APRIL 24 — Recently, Health Minister Datuk Seri Dzulkefly Ahmad shared findings from the 2025 National Health and Morbidity Survey (NHMS). He highlighted that only 14.7 per cent of elderly Malaysians were ageing healthily.
This is worrying considering that by 2048 we will have achieved an “aged society” status with more than 14 per cent of our population aged 65 and above. Among the strategies proposed during the launch included the introduction of long-term care insurance. But even with reform in how we finance long-term care, is Malaysia’s care industry prepared to meet the demand?
What is long-term care insurance (LCTI) for?
LCTI is different from medical insurance. Instead of covering healthcare needs, it helps to cover the high costs of long-term care needs such as paying for a nursing home or care facility.
An example is Japan’s national LTCI which requires everyone above 40 to contribute and is supported by tax funding. The LTCI ensures that those aged 65 and above can have subsidised aged care.
Singapore also imposes a mandatory premium payment on its citizens between the ages of 30 to 67, complemented by government subsidies. Under the LTCI, citizens receive lifetime basic monthly cash payouts that increases over time if they become severely disabled, especially during old age.
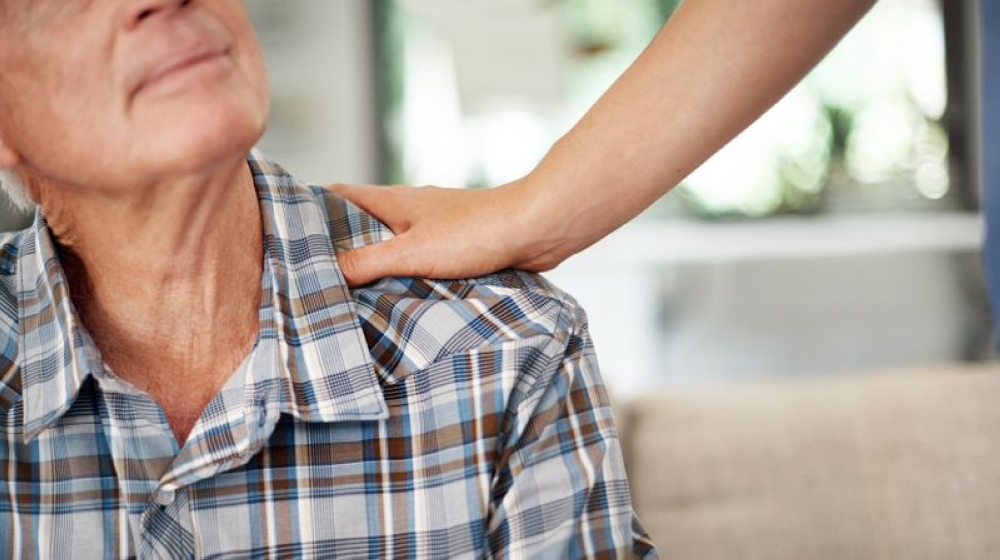
The author argues that Malaysia is unprepared for an ageing population, with gaps in long-term care infrastructure, workforce and affordability requiring urgent, coordinated reforms to ensure accessible and sustainable eldercare. — AFP pic
These LTCI models do not come without flaws. Japan’s LTCI, while providing almost universal coverage, faces escalating costs and its mandatory payment continues even after retirement. Singapore’s broader age group allows for larger scale pooling of funds however it also translates into more people being covered and little is done to facilitate access to service providers.
Malaysia currently does not provide LTCI on its own, although it may sometimes be bundled with traditional life or critical illness insurance policies. The lack of LTCI here may be due to factors including low awareness, premium rates and underwriting standards, high cost in addition to cultural norms that rely on care by family members.
Is our care industry ready?
A paper by the Khazanah Research Institute (KRI), “Care in Malaysia: Emerging Trends, Challenges and Opportunities” has outlined uneven care provisions across the nation and a gap between demand and supply within the care sector.
The paper illustrates that the live-in or residential elderly care centre landscape is highly privatised and small in number, introducing issues of affordability. Previous reports of costs ranging from RM1,500 to RM3,000 for basic care— not including medical care! — would be burdensome for most Malaysian families. A small number of government-run residential centres are concentrated in Peninsular Malaysia and only available for extremely poor elderly with no family.
The high costs may not be entirely a matter of the private sector making profit. Care providers, especially those who seek to be legally registered under the Department of Welfare (JKM) would also be struggling with high costs of operations and registration processes.
Starting in 2025, JKM-registered elderly care centres now have to include an 8 per cent service tax despite providing a welfare service. This is but an example of governance that may deter centres from obtaining registration and operating without regulatory oversight. In 2022, it was estimated that between 700 to 1,000 residential care facilities were unregistered.
Costs could potentially be lowered through enrolment in day-care centres during working hours. These are more numerous and mainly provided by the government. Specifically, these refer to Pusat Aktiviti Warga Emas (PAWE) run by the Ministry of Women, Family and Community Development (KPWKM) and the Kelab Warga Emas (KWE) run by Ministry of Health (MOH).
There are over 190 PAWEs nationwide currently, possibly due to the cost-effectiveness of running these compared to residential facilities. However, PAWEs still face issues of availability— a ratio of 13,530 elderly to 1 PAWE compared to Singapore’s 6,323 elderly to 1 facility of similar role— and accessibility.
Malaysia also faces an issue with undersupply of aged care workers. Limited career pathways, low salaries and labour-intensive work mean not many would choose this career. According to another KRI paper, low- and semi-skilled workers in the social care and residential care sector can only earn up to 50 per cent of what high-skilled workers do.
Demand for care services: Day-care or live-in care?
The obvious split between private-driven residential care centres and government-driven daycare facilities signal Malaysia’s policy shift towards more community-based care and encouragement of ageing in place. The Malaysia Ageing and Retirement Survey in 2019 also found that most Malaysian elderly want to grow old in their own homes. More than 70 per cent of their survey respondents indicated that they were not prepared to live in a care centre.
However, there is still a lot of demand for help from the elderly. In 2022, JKM reported that their Home Help Services (HHS) programme — which delivers at-home care through volunteers — catered to close to 7,000 elderly. HHS volunteers can help to do chores, provide companionship and even bring the elderly to the hospital or clinics.
Day-care centres or HHS are insufficient for those with complex care needs or who require constant supervision. Based on NHMS 2025, more than 80 per cent of elderly lack social support, are cognitively impaired, depressed, unable to perform daily activities independently or have chronic diseases. Thus, there is still a requirement to develop residential care infrastructure alongside strengthening community care.
The ‘sandwich generation’ issue
We should also consider the ‘sandwich generation’, where working adults have to shoulder the responsibility for caring for both young children and ailing parents. In the absence of affordable and accessible options, oftentimes Malaysians must choose between financial strain or dropping out of the workforce to provide care themselves. Based on a 2025 KRI survey, 52.7 per cent of women who had previously worked became homemakers due to caregiving responsibilities.
Malaysia needs to reform its aged care service delivery landscape to meet future needs.
Streamlined governance and reduced fragmentation is needed to encourage providers to expand service delivery and spur the growth of the care market. An all-of-government effort and destigmatisation of care as a welfare issue is also important. Through effective planning of resources as well as synergistic collaboration between government, NGOs and the private sector, the availability and quality of care services can be ensured to meet the needs of the population. We must choose to act now to provide an inclusive and sustainable ecosystem for Malaysians to age with comfort and dignity.
* Ilyana Mukhriz is a Research Associate at the Khazanah Research Institute (KRI). Her work at KRI focuses on public health policy and understanding the care economy in Malaysia.
** This is the personal opinion of the writer or publication and does not necessarily represent the views of Malay Mail.






